12/13/16
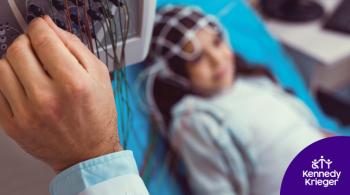
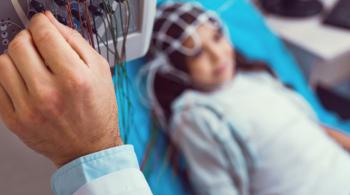
Lisa Carey sat down with Dr. Stacy Suskauer, research scientist and co-director of the Center for Brain Injury Recovery Clinic, to discuss concussion research and how teachers can assist students recovering from mild traumatic brain injuries.
LC: To start off, can you define what a traumatic brain injury is and explain how it relates to concussion?
SS: A traumatic brain injury (TBI) is an injury to the brain caused by an external force. That force may be a result of kids colliding with each other in a football game, an acceleration/deceleration force from a car accident, or a blow to the head from a fall. We distinguish TBI from other forms of brain injury, such as injury caused by insufficient oxygen delivery to the brain or pressure on the brain from a tumor. Within the scope of TBI, concussion is the mildest form. A concussion is a TBI and it is typically distinguished from more severe traumatic brain injury based on duration of alteration in mental status.
LC: What are the different types of symptoms that cause patients come to your concussion clinic?
SS: There are four general categories of post-concussive symptoms:
- Physical symptoms, including headaches, light sensitivity, noise sensitivity, and problems with balance.
- Cognitive symptoms, such as difficulty remembering, difficulty concentrating, feeling foggy, or thinking more slowly than usual.
- Emotional symptoms, with more emotionality, nervousness, irritability, and/or sadness.
- Sleep troubles, typically initially sleeping more than usual but then sometimes having more difficulty with sleep or sleeping less than usual.
LC: For a lot of teachers, myself included, there wasn’t much information available to us while growing up and participating in sports and other activities that might have put us at risk for sustaining a concussion. We weren’t informed of the risk factors, how to treat a concussion, or how serious a concussion can be. I think this causes some confusion when dealing with students who have experienced a concussion. For example, I’ve heard teachers say that we’re being too soft on kids experiencing symptoms and that they should just “shake it off.” What new information would you like to share with teachers about concussion?
SS: We’re learning more and more about concussion all the time. Certainly, concussion is being identified in greater numbers of children. Understanding that a concussion is a TBI is an important starting point. I think it’s also really important to understand that every child experiences each concussion in a different way. While most children will recover from concussion within days to weeks after injury, it is not uncommon for a child to have symptoms for up to a month. Some children will have symptoms that last beyond that period of time. We sometimes hear from children that it seems like teachers expect them to be completely back to baseline within one week after concussion. It would be helpful for teachers to understand that rate of recovery from any TBI, including concussion, is variable. When a child feels supported by his/her teachers, the child experiences less to school-related stress. This seems to help support the child’s overall recovery.
Other key information we have learned about concussion includes the risk of multiple injuries. First, in youth, there appears to be a risk of severe brain injury if another injury to the head is incurred early during recovery from a concussion. While catastrophic “second impact” injuries fortunately appear to be rare, we more commonly see that children who experience a second injury will have a temporary setback in their recovery. In addition, the information developing from professional sports regarding potential later-appearing sequela of repetitive hits to the head is raising awareness about the importance of attending to consussions.
Currently, there are little data on the long-term outcome after concussion in children and certainly that’s an important focus for research.
LC: What are some of the recommendations you send schools when students have prolonged problems following a concussion?
SS: Rest breaks can be really useful for managing symptoms. Taking a brief rest break is usually a more effective way of treating a headache than taking pain relievers. We want the child to have an opportunity to a go to a quiet space for a limited amount of time, approximately 10-15 minutes, but then return to class. We work with the child and the school to identify times in the school day for the student to take breaks, when it’s least disruptive to their learning.
Children tend to work more slowly during recovery from concussion. In addition to needing rest breaks, the child often needs extra time to get work done. Likewise, streamlining assignments, such that a child is only doing essential work, and having additional time to make up missed work are important. You can imagine that if a child has missed some days from school, everyone is anxious for the child to get caught up when they first return, but that is typically not a reasonable expectation when a child is still experiencing symptoms of a concussion.
In order to manage the demands placed on the child and facilitate their success, we often recommend they only be given one test per day once they’ve reached a point in their recovery in which it is appropriate to resume testing. This provides sufficient time for the child to prepare for each test. For older students, coordination is needed among teachers to pace make-up work and tests from all classes in a reasonable fashion.
It is important for each child and family to have a point person at the school. This person functions like a short-term case manager for the student and helps disseminate the needed accommodations and coordinate plans for making up work on a manageable time schedule. The point person should check in with the child daily as they return to school and fade check-ins once the point person, student, and parents agree that the student is making progress in their recovery and has a clear plan for any remaining make up work. Any school staff member who has a good connection with the student can serve in this role.
A child may have difficulty tolerating light and noise, so children really appreciate when the teacher turns the lights off in the room. Managing the noise level in the room can also be helpful. These things not only help with managing the child’s symptoms, but they also show students their teacher understands they need extra support and is trying to help them.
In many situations, the child needs restrictions to their physical activity to prevent a second injury while they are recovering. Early after injury we limit all physical activity, but a recent change in concussion care has been encouraging non-contact aerobic activity when symptoms persist. Research is beginning to show that for children who continue to experience symptoms one month after injury, aerobic activity at a level that does not provoke or worsen symptoms may help speed recovery. Based on this research, many times we request that the school provide the student with an opportunity to participate in non-contact physical activities, such as walking as tolerated.
LC: You mentioned light reduction; a lot of schools are using smart boards and a lot of 1:1 digital devices. Is the glare coming off these devices difficult for kids to tolerate after a concussion?
SS: Some children find digital devices problematic, while others don’t. Many students do report difficulty tolerating prolonged computer time. Sometimes children seem to have more difficulty with quick eye movements or convergence of the eyes (as is needed for close reading) after concussion. Children may find it difficult to move their gaze from the board to their notes. As children who hit their head hard enough to have a concussion also often have a neck strain, frequent head/neck movements can exacerbate pain. If a child is provided with a written copy of notes, this decreases the need to look between the board and their desk, which may help the student better tolerate the classroom environment.
LC: Earlier, you mentioned that many children have increases in emotionality, such as anxiety, due to their concussion. In addition to providing additional time and chunking assignments to reduce memory load, what can teachers do to support the emotional symptoms of a concussion?
SS: Teachers should help students view concussion as a temporary problem that will get better with time and with support to make up missed work. Teachers can help their students by developing a written plan of what assignments have been missed, what assignments are not essential and will be excused, the plan for addressing any missed instruction, and a timeline for making up remaining assignments. A written plan removes the unknown and gives the child a plan to start chipping away at. That’s one way teachers can really reduce student anxiety. The point person should review each teacher’s plan and help identify when adjustments need to be made to reduce overall work load and/or spread out due dates.
I can’t overemphasize the importance of the teacher showing support for the child. Many children feel that since they look normal after a concussion , teachers don’t realize they’re actually still experiencing symptoms. When symptoms persist, students are already feeling frustrated that they are not better yet, so they benefit from school staff showing that they understand the child doesn’t feel like themselves yet. We often joke that if we put a big band aid on a child’s head until they are completed recovered after a concussion, then others wouldn’t question that the child’s brain is still healing. Expressing some compassion can go a long way.