Interdisciplinary Treatment for Individualized Care
From our director, Frank S. Pidcock, MD:

The pediatric orthopedic specialists at Kennedy Krieger Institute are experts in treating congenital, developmental and traumatic deformities of the spine and extremities in children and young adults. At Kennedy Krieger, orthopedics is a true interdisciplinary program, with a team approach for providing individualized treatment designed to meet the needs of each patient.
This close collaboration helps ensure coordination of care and convenience for families. It includes physical and occupational therapists, pediatric medicine and rehabilitation physicians, orthopedic surgeons, genetic counselors, neurosurgeons, orthotists, and seating specialists. Our physicians and therapists work closely with orthopedic surgeons at The Johns Hopkins Hospital, who are widely recognized for their thoughtful, innovative approaches to a wide variety of orthopedic problems.
The story included in this newsletter about Ellie, a patient with Marfan syndrome, is a perfect illustration of how expertise coupled with an interdisciplinary approach leads to the best outcomes for patients. Also in this issue, Ranjit Varghese, MD, director of the Neuromuscular Orthopedics Surgery Program at Kennedy Krieger, answers questions for physicians about single-event multilevel surgery (SEMLS) for children with cerebral palsy. In the Q&A section of this newsletter, he addresses critical questions about the best candidates for surgery, and the best time in a child’s life for the surgery to take place.
Be sure to watch for future issues of Neurorehabilitation Updates for the latest in neurorehabilitation research and treatment options. If you have any questions or would like to learn more about our services, please call our Physician Referral Line at 443-923-9403.
Dr. Pidcock is the vice president of rehabilitation at Kennedy Krieger Institute and director of pediatric rehabilitation in the Department of Physical Medicine and Rehabilitation at The Johns Hopkins Hospital.
Coming Together to Care for Ellie
An interdisciplinary team worked together to help Ellie walk again—and get her life back, too
Surgery is nothing new to Ellie, 13, who has Marfan syndrome, a connective tissue disorder. She’s had numerous bone, heart and eye surgeries throughout her life, but it wasn’t until last year that Ellie followed surgery with inpatient rehabilitation, at Kennedy Krieger Institute. Her three admissions at Kennedy Krieger last year changed her life.
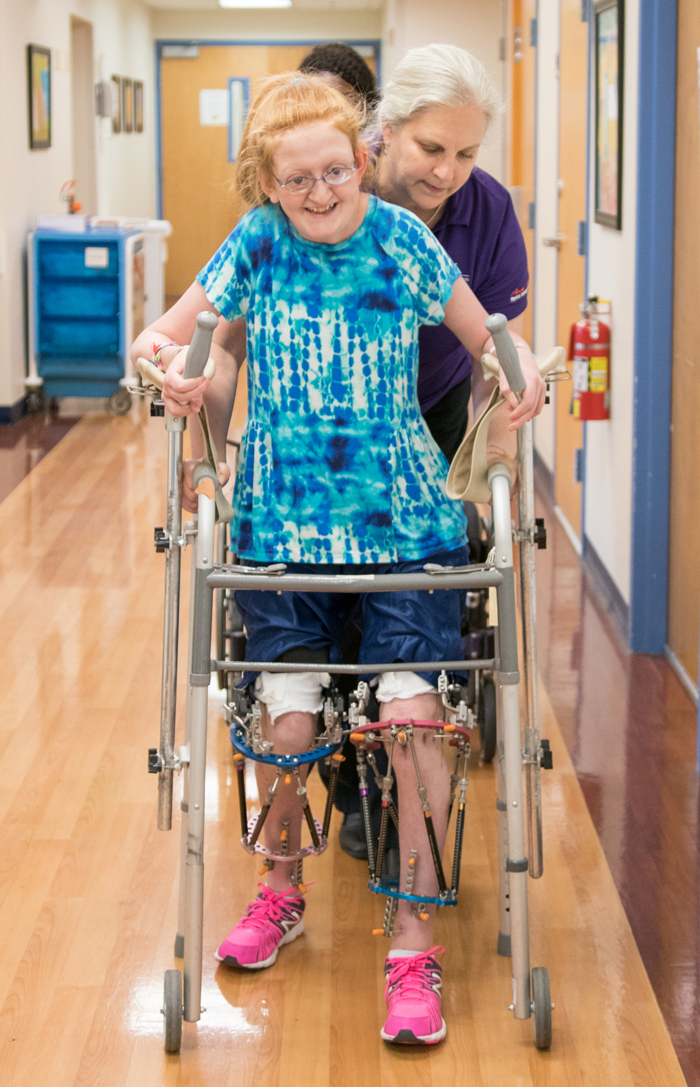
In April, Ellie had surgery at The Johns Hopkins Hospital to correct both genu valgum—“knock knees”—and genu recurvatum, abnormally-shaped knee joints caused by tethered growth plates in the bones of her legs. Ellie hadn’t been able to walk more than a few steps at a time in several years due to the abnormal shapes of her bones and the loose ligaments caused by Marfan syndrome.
To straighten Ellie’s legs, Johns Hopkins pediatric orthopedic surgeon Dr. Claire Shannon cut through Ellie’s femur bones, rotated them, and re-attached them with plates and screws. Then she fitted Ellie’s tibia bones with external ring fixators—metal rings that went around her legs, and which were connected to her bones with pins and wires, and joined together with six telescopic struts.
With the fixators adjusted daily, Ellie’s legs would gradually straighten from their rotated positions. But to walk again, she’d need intense, interdisciplinary and highly specialized inpatient physical and occupational therapies.
“We were hesitant at first,” Ellie’s mom, Becky, explains, “because we’d always done therapy at home. We didn’t really understand what Ellie’s needs would be until after the surgery, and then we realized we couldn’t have handled this at home.”
Ellie and her parents were impressed with Kennedy Krieger from the get-go. “It hit her needs at every level,” Becky says.
“Ellie came here dependent on people for a lot of things, but soon learned she could do many things on her own,” says senior occupational therapist Scott Frampton. He worked closely with Ellie and her family to identify activities that would be fun for her to do while helping her reach her goals.
Working with Heather McLean, inpatient manager for physical therapy, Ellie progressed from bed mobility and maintaining her balance while sitting to standing and walking. “Ellie made daily gains and routinely surprised everyone with her progress,” McLean says.

Ellie also worked with the Institute’s Child Life and Therapeutic Recreation Department, which uses fun activities to help patients fully engage with their treatments. With child life specialist Ali Van Eck, Ellie compiled a special photo album documenting her progress.
At Johns Hopkins, Ellie had cardiac surgery in August, and then surgery to remove the fixators from her legs in October. She followed these surgeries, too, with inpatient rehabilitation at Kennedy Krieger. At the end of the third admission, she was not only moving around with a regular front-wheeled walker, but also beginning to use small base quad canes, and she was able to dress herself for the first time in years.
Throughout all of Ellie’s admissions, Kennedy Krieger staff members ensured that Ellie’s therapies were safe for her to do. “Given that she’d had a major orthopedic procedure while having underlying heart disease”—common for individuals with Marfan syndrome—“we needed to make sure we were not putting too much of a burden on her heart,” explains Dr. Michelle Melicosta, the Institute’s inpatient pediatric hospitalist and Ellie’s attending physician.
At all times, Ellie demonstrated a strong will and drive. Seldom was there a therapy session without lots of laughter and fun, along with hard work, and her effort and attitude always remained at the highest level.
“If Ellie had just gone home” after surgery, Dr. Shannon says, “she wouldn’t have made the gains she has made. It is really remarkable how far her therapists at Kennedy Krieger were able to push her, and how hard Ellie pushed herself—it was well beyond my expectations. It was incredible.”

Q&A: Surgeries that Improve Outcomes in Children with Cerebral Palsy
Q&A with Ranjit Varghese, MD, director of the Neuromuscular Orthopedics surgery program at Kennedy Krieger Institute
When should a surgical intervention for children with cerebral palsy be considered?
We recommend all children with cerebral palsy be examined at 3 or 4 years of age to determine if they would benefit from surgery that would improve motor function. Some of these children would benefit from selective dorsal rhizotomy, which reduces muscle tone permanently. Once muscle tone is reduced, rehabilitation is started. About two years later, the child’s gait is analyzed to determine if orthopedic surgery is needed.
As the child grows, his or her bones may grow abnormally. Selective dorsal rhizotomy doesn’t fix that, so we realign the lower extremities through single-event multilevel surgery (SEMLS). The ideal age for this procedure is between 6 and 9 years old.
What is single-event multilevel surgery (SEMLS)?
SEMLS is a procedure performed on the lower extremities to either improve gait or prevent deterioration in individuals with cerebral palsy. It gets its name from the fact that multiple corrections are made in one orthopedic surgery for soft tissue and bone problems.
What are the benefits of SEMLS?
Results from SEMLS will vary between individuals, but for children with more severe forms of cerebral palsy, as determined by the Gross Motor Function Classification System Level III or IV, SEMLS can help with maintaining existing mobility skills, obtaining independent transfer skills, maintaining stable sitting, and improving lower limb posture and function. For individuals who are non-walkers, benefits will include pain-free sitting and lying down, and improved lower limb posture and function. In addition, making multiple corrections in one surgery results in fewer surgical procedures, reduced rehabilitation time and reduced surgical risks.
What does rehabilitation after SEMLS involve?
Full recovery from SEMLS can take up to one year. After SEMLS, most children will require equipment, assistive devices and new orthotics for a safe discharge home and to begin rehabilitation. Most children will require a wheelchair initially after the surgery, and they may require increased levels of assistance post-surgery. Physical therapy will be needed to work on the following:
- Maintaining or increasing range of motion in the joints.
- Preventing stiffness while healing.
Patients will continue to work with a physical therapist until they reach their pre-therapy goals. We encourage patients to continue regular stretching and strengthening programs, and other exercises like biking or swimming, to maintain strength and conditioning.
Visit the Orthopedic Clinic webpage to learn more about orthopedic programs at Kennedy Krieger, or to make a referral, contact us at FindASpecialist@KennedyKrieger.org or call 443-923-9403.
Kennedy Krieger Welcomes Pediatric Orthopedic Surgeon

Claire Shannon, MD, is a pediatric orthopaedic surgeon at The Johns Hopkins Hospital. She sees pediatric patients from birth through young adulthood who have congenital and childhood skeletal deformities, such as limb length discrepancies, limb deficiencies, skeletal dysplasias, foot deformities and other issues related to abnormal bone growth.
As a pediatric surgeon, Dr. Shannon is skilled at limb lengthening, limb salvaging and similar innovative procedures aimed at improving function with minimal tissue damage.
Epic CareLink is Coming to Kennedy Krieger Institute
Epic CareLink will allow for easy, paperless referrals and automatic follow-up, with nothing to install.

Starting July 1, information about your patients’ care at Kennedy Krieger Institute will be only a few clicks away, with the Institute’s Epic CareLink.
This free, secure, online referring physician portal will enable you to have real-time access to your patients’ electronic health records to track activity such as appointments, lab results, medications and more.
EpicCareLink will:
- Provide 24-hour remote access to view medical records, including procedure notes, reports, clinic notes, medications and lab results.
- Allow you to download and print patient records related to your referral, and manually import patient records into your electronic medical record system.
- Provide immediate and up-to-date information.
- Provide you with a new-patient dashboard giving you a live snapshot of your patients who have recently been admitted to Kennedy Krieger.
- Be customized to what notifications you want to receive about your patients.
- Be compliant with HIPAA. Epic CareLink will also enable you to communicate directly with Kennedy Krieger specialists.
To access a patient’s information, your patient must have been seen by a Kennedy Krieger clinician.
More information about signing up will be available in the next few months. Please email FindASpecialist@KennedyKrieger.org for more information about Epic CareLink.
