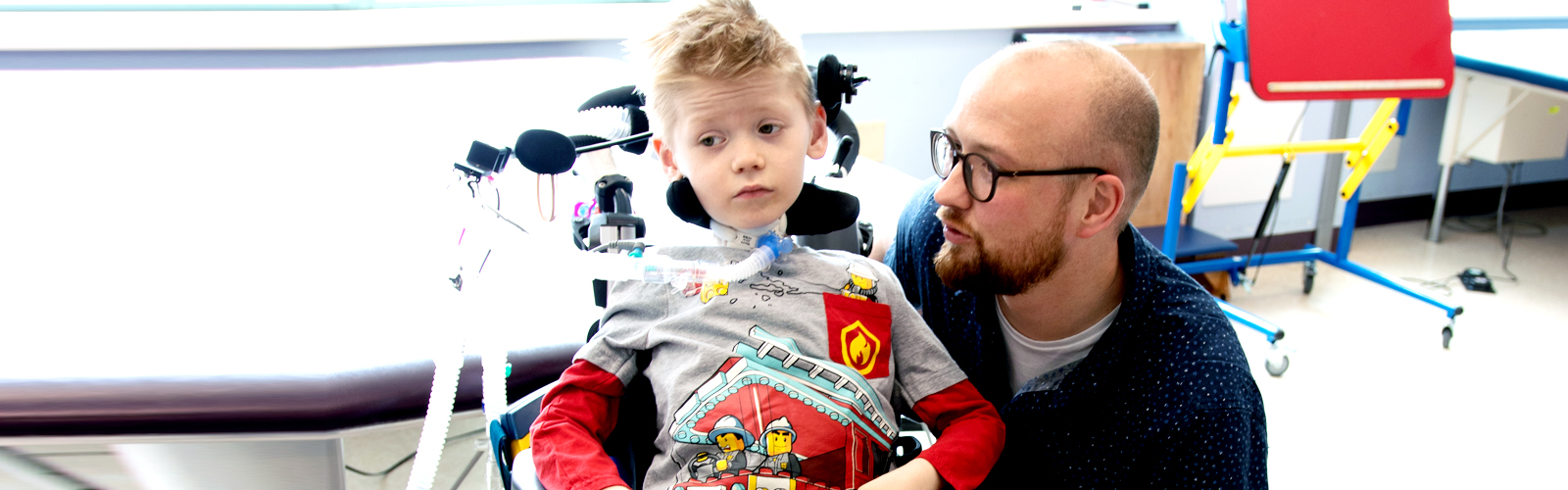
"I can’t hold my head up, and I’m feeling strange,” Geuko told his parents on July 22, 2016.
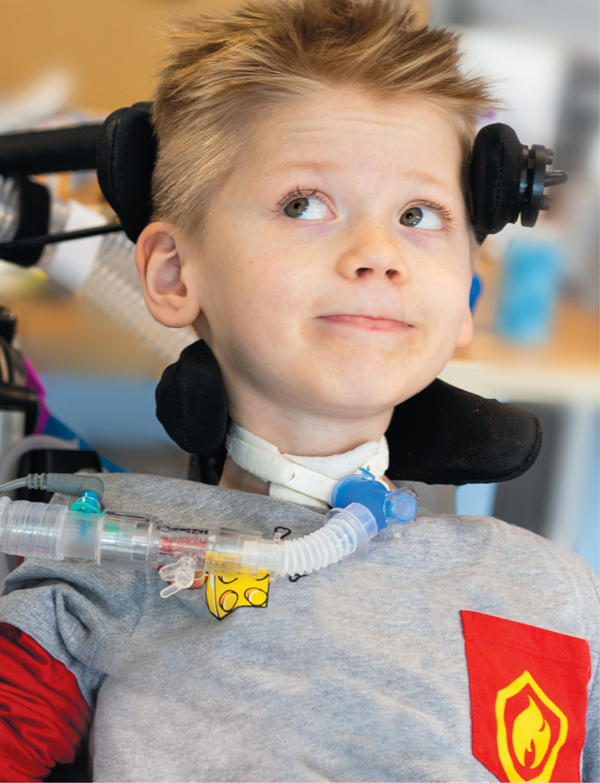
They took him to an urgent care center near their home in the Netherlands. Doctors thought Geuko might have Guillain-Barre syndrome. They sent him by ambulance to the hospital. On the way, Geuko experienced a sudden attack of pain and paralysis and stopped breathing.
“Seeing your almost 4-year-old in a room, intubated, and you don’t know what happened, and he can’t talk—and he was a talker!—lying there…that’s not what you want,” says Gert Jan, Geuko’s dad.
A few weeks later, Geuko became the first person in the Netherlands to be diagnosed with acute flaccid myelitis, also known as AFM.
A Rare, Polio-Like Condition
AFM has likely been around for a long time, but only in the past five years have doctors seen an uptick in diagnosed cases, and more so in even than in odd years. AFM tends to start out with what appears to be a cold, but then develops very quickly into floppy paralysis in one or all limbs, and often an inability to smile, talk or even breathe, explains Dr. Cristina Sadowsky, clinical director of Kennedy Krieger’s International Center for Spinal Cord Injury.
Estimated to affect only one or two in one million people, most of them young children, AFM does not interfere with thinking or sense of feel, explains Janet Dean, nurse practitioner for the center. About 10 to 20 percent of individuals with AFM make an almost full recovery, while others regain only some of the movement they lost. The range of recovery is as varied as the ways in which AFM affects those diagnosed with it. Since 2014, Kennedy Krieger has treated more than 80 children with AFM, “and we learn more about how to treat it with each child we see,” Dean says.

One probable cause of AFM is enterovirus D68. It’s a common virus, usually inflicting no lasting harm, but research suggests it may be causing some people to develop AFM.
After Geuko’s initial illness passed, he was left almost completely paralyzed and on a ventilator. He spent nearly two years at a rehabilitation center in Germany, but what Gert Jan really wanted was to take his son to Kennedy Krieger Institute, which he’d read about online. He’d even gotten in touch with Dr. Sadowsky. In June 2018, Dr. Sadowsky visited Geuko and his family and therapists in the Netherlands.
“Geuko’s family had taken such good care of him, and he’d received good therapy, but what he needed was activity-based rehabilitation therapy,” also known as ABRT, in which Kennedy Krieger excels, Dr. Sadowsky explains.
'All Their Attention to the Kids'
Last February, Geuko and Gert Jan made it to Kennedy Krieger. For three months, Geuko did a combined three to five hours of intense physical, occupational and speech-language therapies a day. Fun activities like crafts and coloring helped him regain movement in his hands. Stretching and strengthening had him sitting up on his own again, walking short distances with a walker and transferring himself, with only minimal assistance, from his bed to his wheelchair—all things he hadn’t done in two and a half years.
“He made phenomenal progress while he was here,” says physical therapist Dr. Courtney Porter. “Our big goal was increasing independence, and that’s exactly what he did.”

Respiratory therapists helped start the process of gradually weaning Geuko off the ventilator. Naturally, Geuko had developed anxiety at the very thought of going off of it. But his therapists went slowly, starting with just a few seconds of decreased support to the lungs for breathing, explains pediatric respiratory therapist Craig Engler. By the time Geuko left Kennedy Krieger, he could breathe for 10 minutes at a time on his own.
Geuko keeps up his therapies at home, and amazes his parents every day with his progress. He can now breathe on his own for more than an hour at a time. Gert Jan hopes to bring Geuko back to Kennedy Krieger for additional therapy, and describes all of the doctors, nurses, therapists and other providers at the Institute as Geuko’s angels, “and the head angel is Dr. Sadowsky. ... They give all their attention to the kids.”
When Breathing Means Freedom
One day in early October of last year, Ava, then not quite 4, suddenly couldn’t move her legs and had trouble breathing. Her local hospital in Maryland sent her to The Johns Hopkins Hospital, where she was put on a ventilator and diagnosed with AFM. Her diaphragm—the muscle that pumps the lungs—was no longer working.

Some children with AFM rely indefinitely on ventilators to help them breathe. But Dr. Sadowsky wondered if a diaphragmatic pacer could reactivate Ava’s diaphragm. The pacers had been used in patients with AFM before, but never to any great effect, and all had been implemented at least six months after paralysis. So Dr. Sadowsky said, “Let’s put this pacer in early, and see if that will help save some diaphragm.”
As soon as the pacer was in, the left side of Ava’s diaphragm started to contract, then expand. Within days, Ava was breathing with decreased support from the ventilator. Her diaphragm had been saved.
But she’d lost her voice, and her ability to move just about every muscle in her body. Four months of intense therapies at Kennedy Krieger’s inpatient rehabilitation hospital helped Ava start to get her life back. Initially, she communicated by fixing her eyes on pictures on a board, explains speech-language pathologist Dana Wanyo. Special tongue and swallowing exercises helped her strengthen her oral and pharyngeal muscles to allow her to swallow safely and speak. Ava speaks with the aid of a Passy-Muir valve, which Wanyo taught her to use to control airflow through her tracheostomy.
In 48 hours, I literally went from having a bouncing 4-year-old to wondering if she's going to make it.”
– Amanda, Ava's mom
Occupational therapist Justine Small helped Ava strengthen her neck muscles to be able to use her head to drive her power wheelchair and use switch-activated toys. “We’re always creatively problem-solving to help our patients become more independent, particularly through play,” Small says.
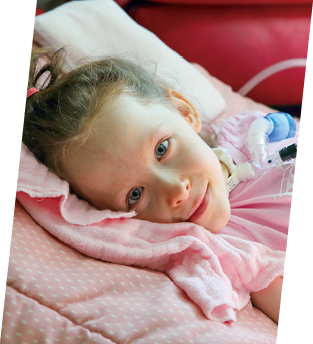
Physical therapist Kimberly Peterson now visits Ava at home through Kennedy Krieger’s Community Rehabilitation Program. To help Ava increase her core strength, they’ll sit on the floor—Peterson supporting Ava with her hands—while playing games or reading books. And while Peterson moves Ava’s arms and legs through their full range of motion, Ava pretends she’s riding a bicycle or doing “ballerina kicks.” To make therapy more enjoyable for Ava, Peterson lets her choose many of the activities they do together.
Now that Ava can talk again, she uses voice-activated technology to do things like turn the lights on and off. “That expands her independence in her home environment,” explains speech-language pathologist Demetria Padussis, who also provides home therapy to Ava through the Community Rehabilitation Program.
And thanks to the pacer, Ava can now breathe with decreased ventilator support for a couple of hours at a time. “At some point, we hope she can be off the ventilator during the day,” Dr. Sadowsky says, “because without the vent—that’s freedom.”
A Strategy for Each Child
Two weeks before Ava developed AFM, Ryleigh, now 4, came down with a cold and then, four days later, with paralysis. She did inpatient and outpatient therapy in Virginia, where her family was living at the time, and started intensive inpatient therapy at Kennedy Krieger in June.
She made excellent gains in using her legs and left arm, “but we weren’t seeing any significant improvements in her right arm,” says Dr. Michelle Melicosta, medical director of the Institute’s inpatient rehabilitation hospital.
Dr. Melicosta and her colleagues suspected Ryleigh might benefit from nerve transfer surgery, in which segments of healthy nerves are transferred to the nerves that aren’t working, to reinvigorate them. The surgery took place at Johns Hopkins on July 15, and it’s hoped that Ryleigh will start to get more motion back in her right arm by early next year.

Because AFM can change a child’s life so abruptly, and the therapies that children with AFM do are so intense, pediatric psychologists usually step in to help children understand and cope with what’s happening. “Distress and anxiety are common in this population,” says pediatric psychologist Dr. Margaret Tunney. “It’s to be expected. Their ability to move their body has changed very quickly, and they are doing a lot of very difficult tasks.”
They're resilient kids. It's exciting to see the progress they make.”
– Dr. Courtney Porter, physical therapist
Dr. Tunney and her colleagues develop individual strategies for each child to help them participate in therapies and meet their goals. They often join physical, occupational and speech-language therapy sessions to implement child-friendly strategies to maximize rehabilitation potential. Dr. Tunney worked closely with Ryleigh’s therapists and mom, Mallory, to learn more about Ryleigh and develop an individualized program for her therapy sessions.
During her eight-week inpatient admission, Ryleigh increased the distance she could walk with a walker from 150 to 300 feet—the length of a football field. This past fall, she started outpatient therapy three days a week at Kennedy Krieger, still following the special program Dr. Tunney created for her.
“She’s doing amazing!” Mallory says. “The amount of confidence she’s gained since going to Kennedy Krieger has been out of this world!” Instead of doubting herself and her abilities, Ryleigh now trusts herself in what she can do. “That’s made all the difference in her gaining back some of her independence.”
It’s successes like these that give children with AFM and their families hope and a reason to stick to their therapies. As the victories add up—two steps becoming four, five minutes off the ventilator becoming an hour, tiny head or toe movements activating a wheelchair—a new vision of independence starts to come into focus. And that’s the ultimate reward for all of their hard work.
Support Us in our Fight
Need assistance? Contact us at HelpKids@KennedyKrieger.org or (443) 923-7300. Your donation is greatly appreciated.
The Kennedy Krieger Foundation is a 501(c)(3) nonprofit organization.
EIN: 52-1734695