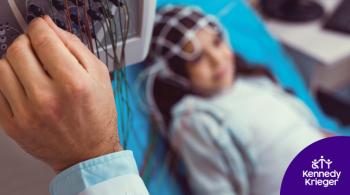
Kennedy Krieger Institute's researchers are leaders in the worldwide effort to prevent and treat disorders of the brain, spinal cord, and musculoskeletal system.
Learn More About Our Research
Intellectual and Developmental Disabilities Research Center (IDDRC)
Our center is central to a scientific enterprise involving hundreds of investigators working to understand and address the problems of developmental disabilities.
Clinical Trials
Breaking New Ground in the Understanding and Treatment of Life-Altering Neurological Disorders
Participate in Research
Kennedy Krieger’s scientists and researchers have made crucial discoveries, leading to innovative treatments, enhanced diagnosis, patient care and student education for individuals with disorders of the nervous system. This work is possible because of our research participants, who play a pivotal role in helping make new discoveries.

Centers, Labs & Research Cores
Kennedy Krieger's scientists and researchers are leaders in the worldwide effort to prevent and treat disorders of the brain, spinal cord, and musculoskeletal system.